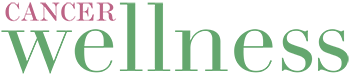My journey began with severe abdominal pain in March 2018. It lasted for an entire weekend. The pain was gone by Monday. I was 54 years old and had been living in Southern California since I was 21.
By early May, the severe pain returned. Now, I was concerned so I phoned my primary care physician to request an exam. My last physical had been in Sept. 2017. My physician ordered an MRI based on the exam and when the MRI results arrived two days later, she referred me to a gynecologist for an ultrasound. Within two weeks, I heard the news—I had two large masses on one of my ovaries the size of a football.
I calmly asked if this would be outpatient surgery. “Sadly, no,” the gynecologist firmly replied. “These are too big for me to take out with the da Vinci method. I’m referring you to schedule a consultation with a gynecological oncologist.” WHAT?!
I did not have a good experience with her referral and began my own research. I chose the GYN/ONC center within City of Hope in Duarte, Calif. knowing about its stellar reputation from working in the California healthcare industry for 17 years. City of Hope is a research hospital and the staff knew that would be to my advantage as well as knowing my PPO insurance had them listed as in-network. So many people facing life-threatening disease find their insurance may limit choices for care.
It was during that initial consultation with the gynecological oncologist in late June that I heard the word “cancer” for the first time. Cancer? ME?
I politely said, “I want you to know from the start that I am not interested in having chemotherapy no matter what the stage of the tumors.” The doctor looked up from his clipboard and said, “Well, it’s too early to know what stage. I don’t advise you to make a rash decision about chemotherapy now. If we don’t insert a chemo port during surgery, and you change your mind, we’d have to do a second surgery.”
Receiving a consultation and hearing the word “tumors”—and “cancer”—made me emotional. Learning I may need not just one surgery but possibly two was terrifying. I had never had a major surgery. I agreed to the port and signed the papers.
The next couple weeks brought a contrast CT scan, a blood draw and an EKG—all the normal pre-op tests. During another consultation after these tests, my oncologist said, “I see you’ve been scheduled for surgery Aug. 6. Did you choose that date?”
“No, a scheduler phoned me and asked if that date was okay,” I said.
“Let me check on something and I’ll be right back,” he replied. He came back to the examination room and said, “Let’s choose July 23. Is that okay with you?” I now had less than two weeks until surgery.

As I left the appointment, I thought to myself, “Wow, how ironic? I’m having major surgery just two months to the day of my MRI revealing the tumors on my ovary.”
I chose to tell only close friends of my situation. One evening, my brother’s best friend called me after learning about my upcoming surgery. He is a throat cancer thriver. His encouragement and love were very helpful and insightful. “Remember you are more than this diagnosis,” he said. “This is happening to your body, not to you, the person.” Those words resonated so deep that I often meditated on them throughout my first year of recovery.
The seven-hour surgery was more intense than we originally expected. Besides a full hysterectomy, my spleen and omentum lining were removed, my diaphragm was scraped and two inches were cut from my liver.
On my third day in the hospital, I learned I had stage IIIC ovarian cancer. A projected seven-day stay in the hospital turned into three weeks due to complications from double pneumonia and an infection in my incision. I had trouble getting all my organs to “wake up” during my hospital stay. These were not the things anyone warned me about prior to surgery. No one informed me I’d be woken up every four hours, only sleep on my back, have three IVs attached, receive two shots in my stomach everyday to help avoid blood clots and wear compression boots on each leg.
My mom was with me everyday for 12 hours at a time. She stayed at a nearby hotel and extended her stay twice. My mom, brother and close friends’ encouragement was a huge help to my journey the first year. They showed up and were selfless and strong when I was weak.
Your days take on a whole different routine in a hospital. You are awakened every four hours for vitals, a daily 5 a.m. blood draw and a daily first round visit around 6:15 a.m. from a hospitalist. After three weeks in a hospital, you get familiar with the staff on rotation. I met some wonderful people who genuinely cared for my emotional and physical healing.
Because I had agreed to having a chemo port placed during surgery, I tried after discharge to schedule the outpatient surgery to have it removed. However, at both post-op appointments with my oncologist, it was clear they weren’t going to schedule to remove it until I met with the head of the chemo department.
I didn’t tell my surgeons that I was going to a wellness center for two weeks in San Diego early September. Because of my decision, pre-surgery, to start following a plant-based food plan, my brother and best friend learned of Optimum Health Institute in San Diego (OHI). My brother graciously paid for my two-week stay. I went a month after discharge.
During my stay, I truly learned that the saying “food is medicine” is not a cliché. OHI holds three classes a day and, though optional, the classes and “teachers” give you a roadmap to follow. Most of the teachers shared their personal “health opportunity” that led them to OHI prior to becoming either a volunteer or teacher. I learned again how your thoughts and words are powerful. From that time on, I chose to refer to my ovarian diagnosis as a health opportunity and rarely said the word cancer.
OHI also offers lymphatic exercise twice a day, daily mediation and an evening class. The class topics include Tools for Change, Mental Detox, Food Combining, and Communication, among others. You are totally unplugged at OHI and it was freeing to have that atmosphere of nature and calmness. Though it is nestled in a neighborhood suburb of San Diego, it is quiet and ideal for reflection of each day’s classes. I met so many kind and interesting people with varying circumstances which led them to OHI.

I gained knowledge that I work to incorporate in my life every day to be a better version of myself. Choosing a plant-based diet is only part of my healing—I came out of OHI with tools to assist me in healthy life choices. In addition to going from a vegetarian food plan to vegan, I changed beauty and cleaning products to natural/vegan and went to acupuncture for four months. What I learned there reinforced that my choices are the right choices for me.
My appointment with the head of the chemo department was the Monday after I got home from OHI. During the appointment, she asked a variety of questions and ultimately said, “Without chemotherapy, you won’t make it to Christmas.” This was September. I told her while I appreciated her expertise, I was going to embrace a more holistic approach. The chemo port surgery was scheduled three weeks later.
In late November of 2018 I had another contrast CT scan, blood draw and upcoming appointment with my doctor. The results were fantastic!
“Your blood draw shows your CA-125 at 7.3 and we find nothing alarming in the contrast CT,” the doctor said. “We will continue to monitor you with blood draws every three months until Sept. 2020 and if you have any severe pain or other symptoms, I will then want to do another contrast CT scan.”
At my September 2019 check up with my doctor, my blood draw results of the CA-125 marker was a win again. I had a score of 10.4, well within the range to stay below 37. I was so overjoyed. I could not contain my tears and hugged him and said, “Thank you for saving my life.” Though my birthday is actually in September, I felt like this was a NEW birthday!
I made the decision in Aug. 2019 to move back to my home state of Illinois for family reasons and arrived in late October. As I settled back into the area, I wanted to find a support group. I had found two on Facebook, but I knew coming back to the suburbs after leaving at age 21 meant I didn’t have a huge circle of close friends like the “tribe of sisterhood” I had in Southern California for more than 30 years.
I found the National Ovarian Cancer Coalition (NOCC) by searching for a support group. I was thrilled there was one so close and attended their first 2020 Illinois chapter meeting in January. The chapter presidents Karen [Young] and Sandy [Cord] were so welcoming. It was wonderful to meet other thrivers. Each thriver shared a brief summary of their own journey. We learned all the ways the local chapter supports newly diagnosed patients and thrivers, and I immediately signed up at the end of the meeting to help on a couple of committees.
Now, two years later, I want to be a beacon of hope like other women have been to me from the Illinois NOCC support group. If sharing my story can help one woman get diagnosed earlier than I did, I will be honored.
My best advice is to do research on your diagnosis and make choices for a plan of care that you want from a cancer diagnosis or other chronic diagnosis. I went “against the grain” and chose to NOT have chemotherapy as part of my plan of care. I celebrated my two years of remission recently with an open heart of gratitude and optimism for my life. Every day, I strive to give more love, stay in the moment, be grateful and show kindness always.